Making basic comparisons between the numbers of COVID-19 positive tests or deaths across different geographic regions using raw figures may seem straightforward. But coming to conclusions about the significance of differences is fraught with difficulty, given differences in population structures (particularly age).

This explainer builds on our outline article and looks at the wealth of data and the charts behind recent reports from the Department of Health (DoH) and Northern Ireland Statistics and Research Agency (NISRA). Those organisations present a standardised analysis of COVID-19 infections (positive test results), hospital admissions and deaths, to assess the different health outcomes across regions of Northern Ireland, with a particular focus on areas of least and most deprivation.
The DoH analysed surveillance data up to 26 May 2020, while NISRA focused on deaths between 1 March and 31 May 2020. Back in April, FactCheckNI published several articles about death rates.
A comparison of mortality rates across England, Scotland, Wales and Northern Ireland (for March and April) was recently published by the Office for National Statistics (ONS). (Note that the ONS data were annualised – assuming the rate of deaths during March and April would prevail over 12 months – unlike the three-month figures produced by NISRA.) ONS also published mortality rate analysis by relative deprivation for England and Wales, and reports on how mortality rates vary by ethnicity and religion.
Age-standardised rates for infection, hospital admission and mortality have been adjusted to take into account underlying differences in population structure (age and sex) relative to a standard ‘reference’ population. These adjustments allow valid comparisons to be made between geographical areas.
Summary
- Males in older age groups have a proportionately higher COVID-19 mortality rate than females.
- The 10% most deprived areas of Northern Ireland have the highest standardised infection rate (COVID-19 positive tests), the highest standardised hospital admission rate, and the highest standardised mortality rate for COVID-19.
- The infection rate of over 65s is highest in the most deprived decile in Northern Ireland (and more than 70% above Northern Ireland average).
- In terms of council areas, Belfast has the highest COVID-19 related mortality rate, and Fermanagh and Omagh the lowest.
- The mortality rate for COVID-19 is higher in urban areas than rural areas.
- Northern Ireland had the lowest mortality rate of the four UK nations for deaths involving COVID-19 in March and April 2020, while England had the highest rate.
- ONS suggests differences in COVID-19 risk of death between ethnic groups (in England and Wales) not all explained by social-economic disadvantages.
- Looking across from most to least deprived areas in the Republic of Ireland and Northern Ireland, mortality rates do not follow the gradient of decline in England, Wales, and Scotland.
Sex
The DoH found that the age-standardised infection rate (based on positive tests for COVID-19) was a third higher in females (308 cases per 100,000) than males (234 cases per 100,000).
Of individuals who tested positive, just over a quarter (27%) were admitted to hospital for treatment, with positive tested males twice as likely to be admitted (39%) as females (19%).
The age-standardised admission rate of patients admitted to hospital with confirmed (positive test) or suspected COVID-19 (clinical diagnosis) was nearly a third higher amongst males (494 per 100,000) than females (383 per 100,000).
Between 1 March and 31 May 2020, 385 deaths of females in Northern Ireland were related to COVID-19 (derived from information on death certificates and including people not positively tested) and 379 deaths of males. During the same period, there were an additional 1,943 non-COVID-19 related deaths of females and 1,745 of males.
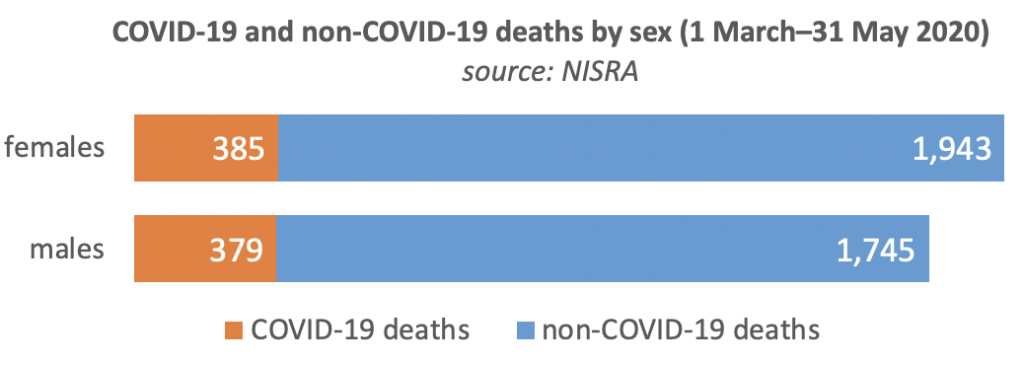
NISRA explains:
“The number of deaths occurring in a population is useful for determining the magnitude of a public health problem. However, mortality rates are used when making comparisons between population groups (for example, comparing males and females or geographies) or when comparing trends over time. Mortality rates are a measure of the frequency of occurrence of death in a particular population at risk during a particular time period.”
NISRA uses age-specific mortality rates – known as ‘crude rates’ – to allow comparison between specified age groups (in wide age bands). They show the number of COVID-19 related deaths per 100,000 population at risk.
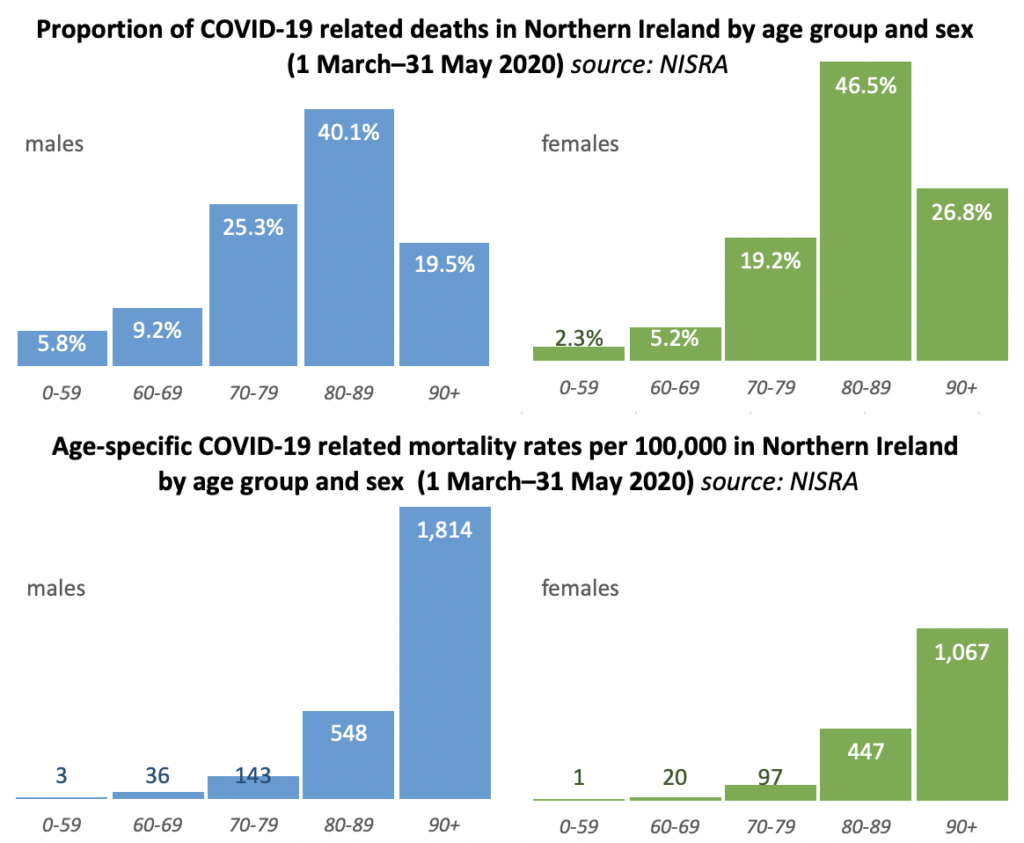
The top charts show the breakdown of overall COVID-19 related deaths by age group and sex.
The lower charts use the age-specific mortality rate, which takes into account the fact that there are fewer males than females in the older age groups in Northern Ireland, and shows the true risk of death.
Males in older age groups have a proportionately higher rate of death from COVID-19.
Council Area
A population with a greater proportion of older people is expected to have more deaths per population.
The usual address of the deceased as recorded on the death certificate allows deaths to be compared across local government districts (LGDs). The use of age-standardised mortality rates (ASMRs) takes into account the differences in age profile of the different LGDs.
Belfast has the highest COVID-19 related mortality rate (per 100,000) at 81.1 (using data up to 31 May 2020). Antrim and Newtownabbey is next highest at 64.4. Fermanagh and Omagh is lowest at 16.2. The comparable figure for all of Northern Ireland is 48.2 COVID-19 related deaths per 100,000 population.
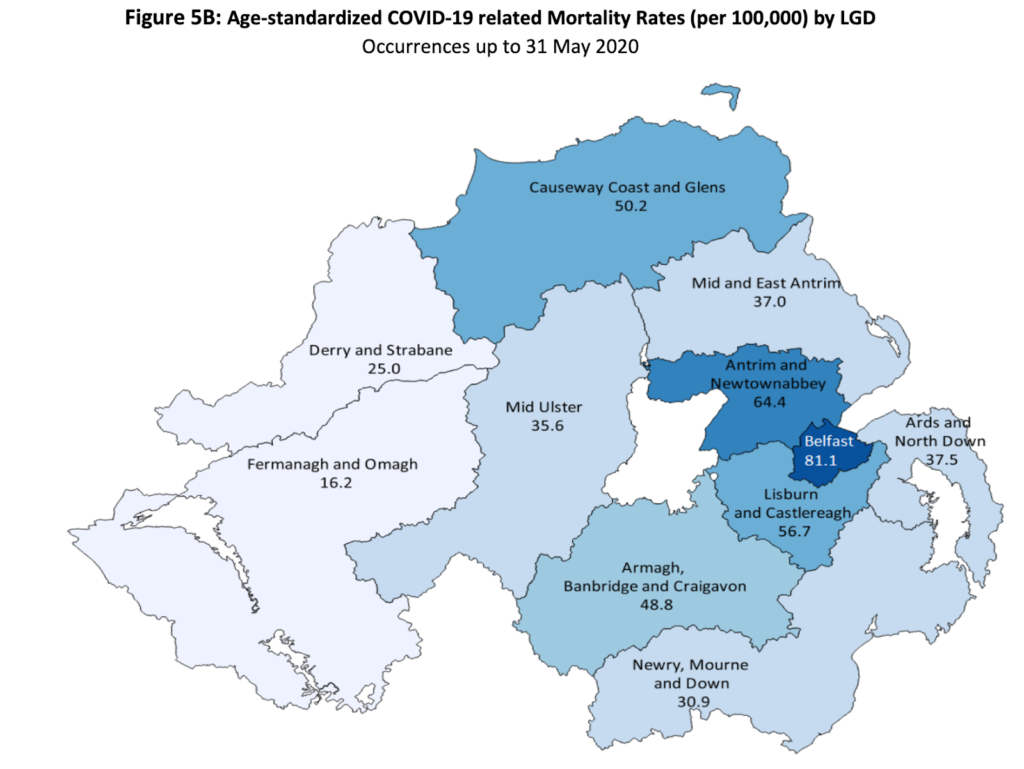
The DoH did not break down infection rates and hospital admission rates by LGD.
Areas of Deprivation
The Multiple Deprivation Measure (NIMDM2017) combines seven separate domains of deprivation into an overall summary measure representing an area’s relative disadvantage. (England, Scotland and Wales use different deprivation measures that are not directly comparable to Northern Ireland.)
The DoH assigned individuals who tested positively or were admitted to hospital to one of ten deciles, ranging from the most deprived to the least deprived, based on provided address information.
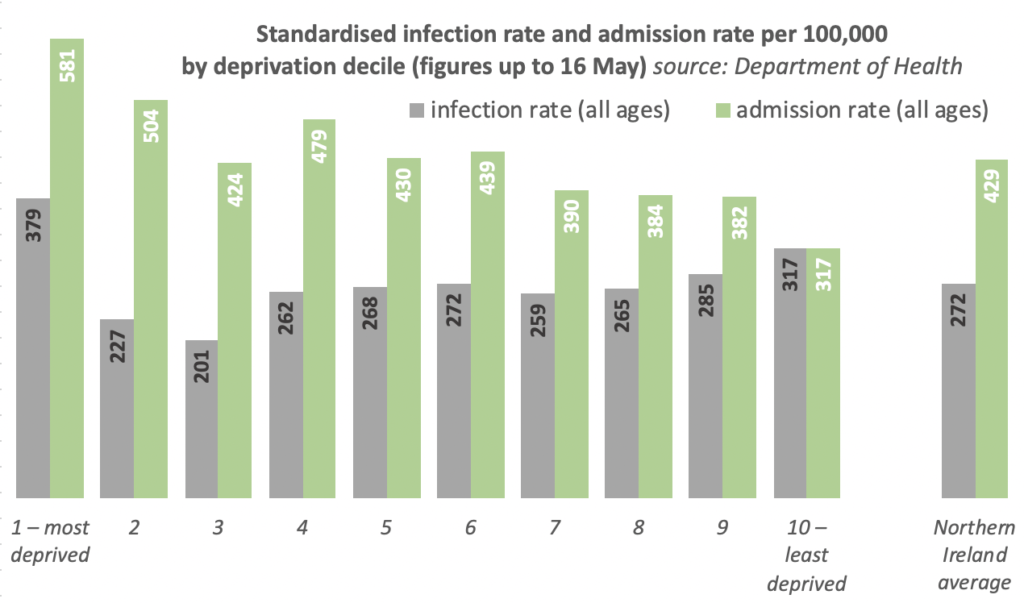
DoH found that the standardised infection rate (grey bar in chart above) is highest in the 10% most deprived areas of Northern Ireland (379 cases per 100,000), 40% higher than the Northern Ireland average (272 cases per 100,000), and 20% higher than the least deprived decile (317 cases per 100,000).
The DoH report warns that “there may be factors other than deprivation that contributed to the observation [that COVID-19 infection rates were highest in the 10% most deprived areas of Northern Ireland] such as occupation and/or population density. This may also be important to note for the 10% least deprived areas where infection rates were also relatively high.” For reference, 89% of the population in the 10% most deprived areas and 96% of the population in 10% least deprived areas live in urban areas (as opposed to urban/rural mixed or rural areas).
Standardised admission rates for patients admitted to hospital with confirmed or suspected COVID-19 was highest in the 10% most deprived area (581 per 100,000), 35% higher than the Northern Ireland average, and 86% higher than the 10% least deprived area (317 per 100,000).
While the least deprived decile had a relatively high standardised infection rate, its standardised admission rate is the lowest of any decile. In general, the infection rate gradient (people who tested positive for COVID-19) is not consistent across the deprivation deciles, while the hospital admission rate trends downwards from most deprived to least deprived decile.
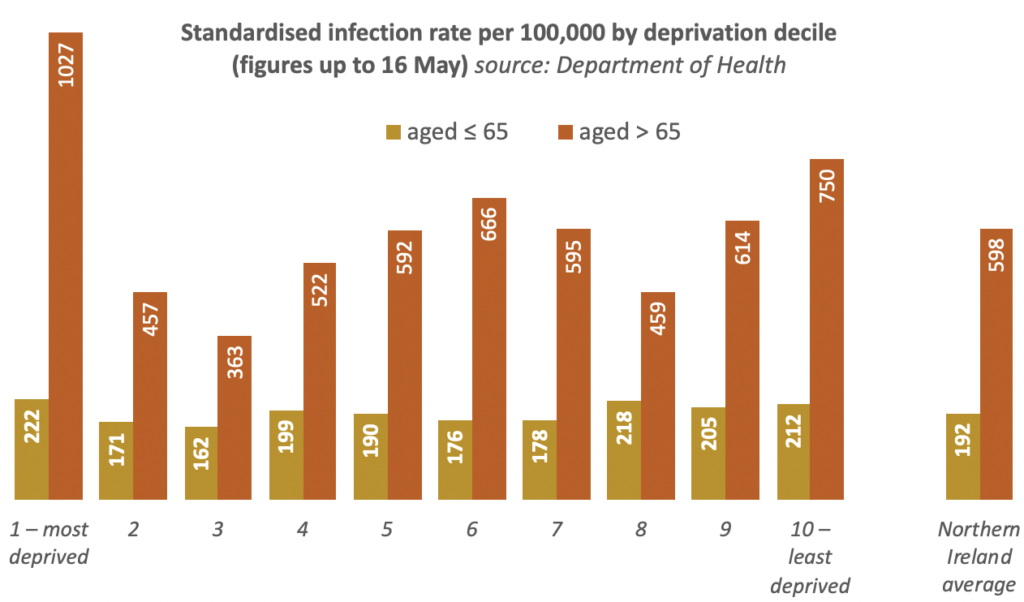
When the infection rate is further divided into those aged over 65 and those aged 65 or under, the differences become even more stark, with the infection rate of over 65s highest in the most deprived decile (1,027 per 100,000), more than a third higher than the least deprived decile (750), and over 70% higher than the Northern Ireland average for over 65s.
Whereas the DoH used deciles, NISRA assigned individuals who died with COVID-19 to one of five quintiles, using the usual address of residence recorded on death certificates.
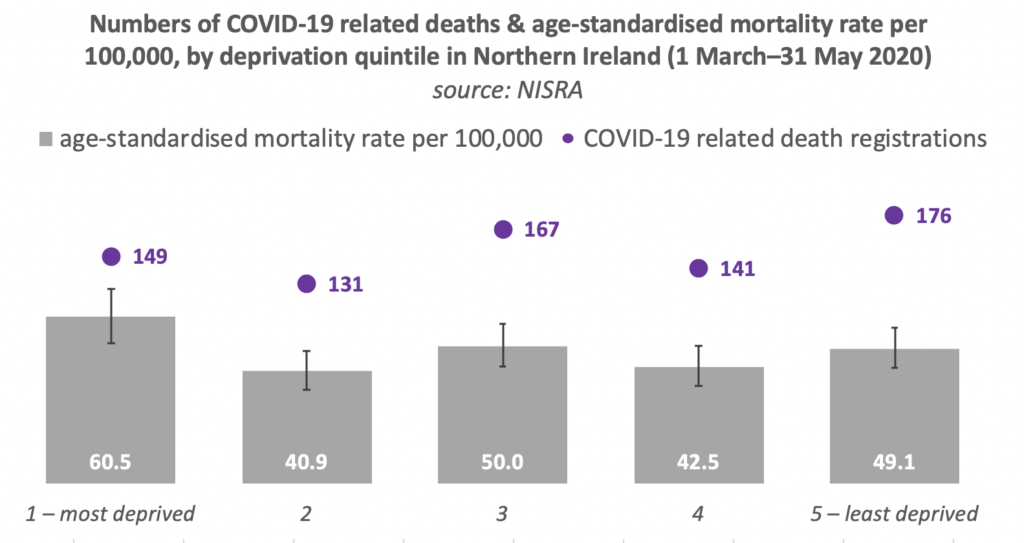
NISRA notes that “the relatively low mortality rate in quintile 2 compared to all other quintiles is not found when looking at non-COVID-19 mortality” and “care should be taken when comparing this decrease due to the wide confidence intervals”.
The mortality rate for COVID-19 is highest in the most deprived areas of Northern Ireland, while the actual number of COVID-19 related deaths is largest in the least deprived areas.
Urban vs Rural
NISRA used the 2015 Statistical Classification and Delineation of Settlements to categorise Northern Ireland’s 890 Super Output Areas as urban, rural or urban/rural mixed. (DoH’s exact methodology for categorisation is unclear.) Note that in the chart below, DoH’s figures include cases up to 26 May 2020 and use the 2018 Mid Year Estimate (MYE) of population, while NISRA includes deaths 1 March–31 May 2020 and uses 2019 MYE.
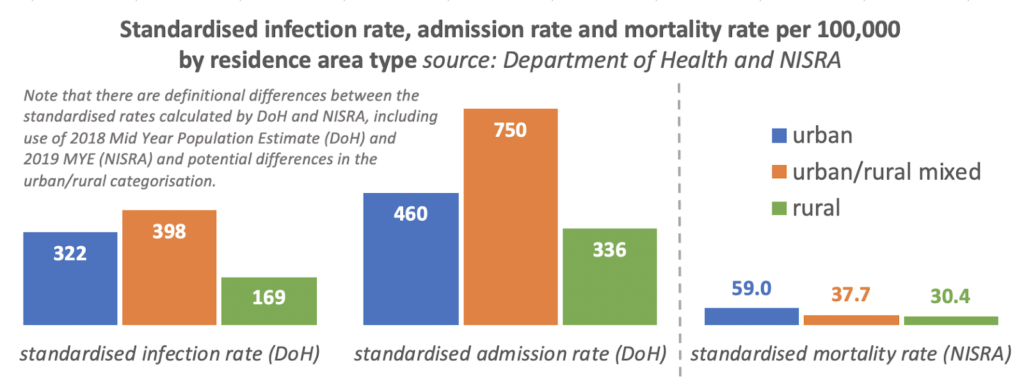
Standardised infection rates (positive tests for COVID-19) were markedly higher in urban/rural mixed areas, and lowest in rural areas (just over half of the urban rate of infection).
Standardised admission rates (for individuals with confirmed or suspected COVID-19) were again highest in urban/rural mixed areas, and more than double admission rates in rural areas.
This pattern of infection and admission rates was not found in mortality rates. NISRA found that the mortality rate for individuals living in urban areas (59.0 per 100,000) was nearly twice as high as those living in rural areas (30.4 per 100,000), and 56% higher than those in urban/rural mixed areas (37.7 per 100,000). The Northern Ireland average was 48.2 per 100,000).
Comparisons across the UK
An ONS report showed that Northern Ireland had the lowest age-standardised mortality rate of the four UK nations for deaths involving COVID-19 in March and April 2020, while England had the largest of the four nations.
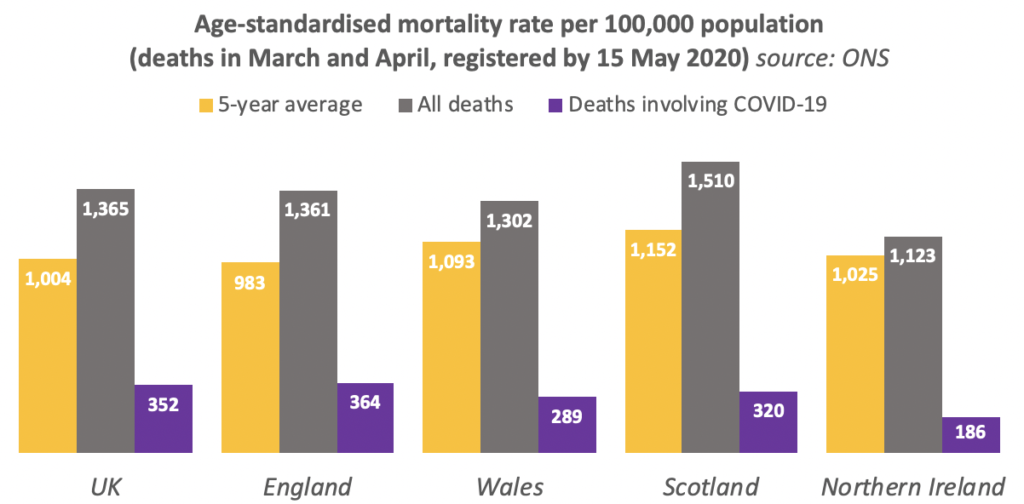
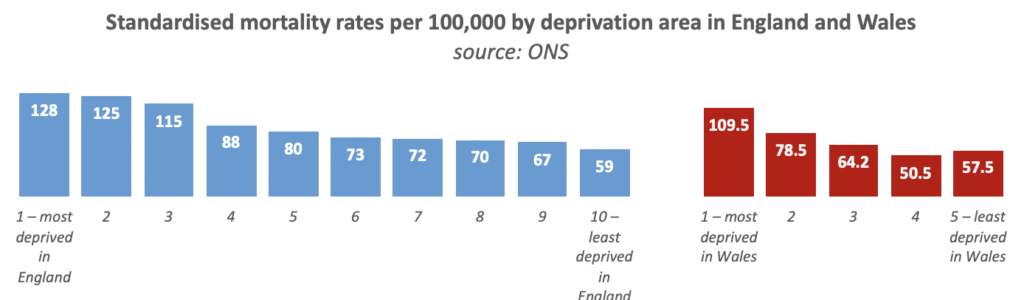
ONS also produced separate statistics for age-standardised mortality rate per deprivation deciles in England and per deprivation quintiles in Wales. While the deprivation measures are not directly comparable between England and Wales, or with Northern Ireland, the figures show a steady decline in mortality rate through the deciles from the 10% most deprived areas to the 10% least deprived areas in England, and a similar (but not absolute) trend in Wales.
Statistics published by National Records of Scotland show that the age-standardised rate of deaths involving COVID-19 for males was higher than females in each of March, April and May this year. The rate for males across March–May (366.5 per 100,000) was 45% higher than the rate for females (252.6 per 100,000).
The mortality rate for those living in the 20% most deprived areas of Scotland (118.9 per 100,000) was 2.1 times higher than the 20% least deprived areas (57.6 per 100,000). The report notes that the mortality rate for all deaths in this same period in the most deprived quintile is 1.9 times higher than the least deprived quintile. The mortality rate for deaths involving COVID-19 steadily decreases in each quintile from most deprived to least deprived.
Another ONS report compared COVID-19 related deaths by ethnic group (2 March–10 April in England and Wales). Adjusting for age, they found that the death rate among Black females was 4.3 times higher than White ethnicity females, and 4.2 times higher when comparing Black males with White ethnicity males.
After taking account of additional factors – socio-demographic characteristics and measures of self-reported health and disability using 2011 Census figures – ONS found that the risk of a COVID-19 related death for males and females of Black ethnicity reduced to 1.9 times more likely than those of White ethnicity. Similarly, males in the Bangladeshi and Pakistani ethnic group were 1.8 times more likely to have a COVID-19-related death than White males when age and other socio-demographic characteristics and measures of self-reported health and disability were taken into account; for females, the figure was 1.6 times more likely.
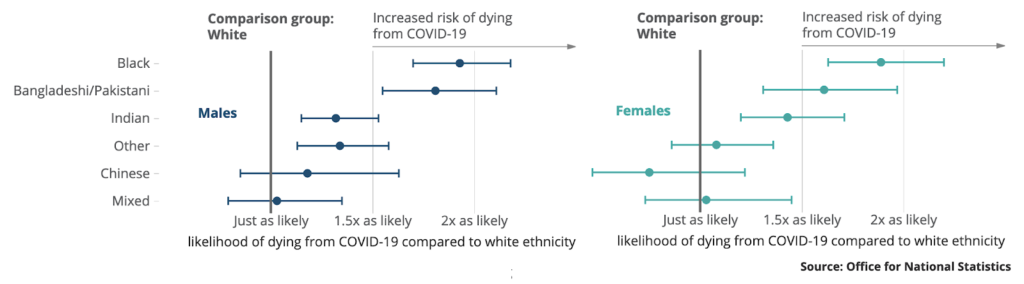
ONS concluded that [for England and Wales] “these results show that the difference between ethnic groups in COVID-19 mortality is partly a result of socio-economic disadvantage and other circumstances, but a remaining part of the difference has not yet been explained”.
A further ONS report assessed the variation in the rate of death involving COVID-19 between self-identified religious groups (including “no religion”) using deaths in England and Wales between 2 March and 15 May. The age-standardised mortality rate (ASMR) for males in Muslim and Jewish religious groups was more than double that of Christian males or males with no religion. The ASMR for females in Muslim, Jewish and Hindu religious groups was just under double that of Christian females, and around double of females with no religion.
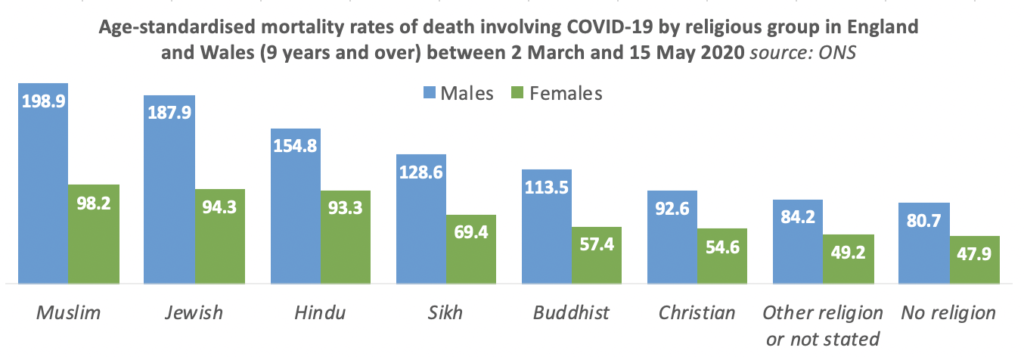
As well as age-standardisation (green in the chart below), ONS went on to make further adjustments for population density, region, rural and urban classification, area deprivation, household composition, socio-economic position, highest qualification held, household tenure, household exposure, and self-reported health and disability. The fully adjusted results (in blue below) show differences in risk between religious groups that are specific to those religious groups and are unlikely to be associated with any of the factors listed earlier.
Comparisons across the island of Ireland
Ireland’s Central Statistics Office (CSO) issued a bulletin examining infection and mortality statistics between 22 February and 22 May 2020. Their analysis used data provided by the Computerised Infectious Disease Reporting (CIDR) through the Health Protection Surveillance Centre. These statistics about deaths are not based on information on death certificates – the long death registration period in the Republic of Ireland means these data are not yet guaranteed to be available – so CSO’s report is not directly comparable with the publications from the Northern Ireland Department of Health or NISRA.
The definition of deprivation used in the Republic of Ireland differs from Northern Ireland. Cases of infection or death were assigned to one of five quintiles (20% bands).
The Standardised Confirmed Incidence Rate (SCIR) adjusts the rate of incidence of COVID-19 (by positive test) using a standard age distribution. The SCIR for the least deprived quintile was 606 per 100,000 population, 14% higher than the confirmed incidence rate for all areas (532 per 100,000) and 31% higher than the incidence rate in the most deprived quintile (462 per 100,000).
The standardised incidence rate was higher for females (603 per 100,000) than males (459 per 100,000). The mortality rate was higher for males (30 per 100,000) than females (27 per 100,000).
The Standardised Death Rate (SDR) of the most deprived quintile (30 per 100,000 population) was lower than the least deprived quintile (35 per 100,000), both extremes higher than the national average (29 per 100,000). In four out of five quintiles, males had a higher mortality rate than females.
Examining the mortality rates across areas of different relative deprivation in the Republic of Ireland and Northern Ireland shows that the patterns do not follow the English, Welsh and Scottish gradient of decline from most deprived area to least deprived area.
FactCheckNI is Northern Ireland’s first and only dedicated independent fact-checking service and a verified signatory to the International Fact-Checking Network’s Code of Principles. You can learn more about about FactCheckNI, our personnel, what our article verdicts mean, and how to submit a claim.




