“Seasonal flu” is a very common illness, and tends to be more severe than the common cold. The most common symptoms are a sudden high temperature, sore throat, cough, headache, tiredness and general aches and pains. Flu can also cause nausea, loss of appetite, a runny or blocked nose, sneezing, and cause you difficulty sleeping. The World Health Organisation explains that “in temperate climates, seasonal epidemics occur mainly during winter, while in tropical regions, influenza may occur throughout the year”.
Does a cold count as seasonal flu?
While the symptoms are similar, colds and flus are distinct. Colds and flus are caused by different viruses. Flu is caused by one of four types of influenza viruses, while there are three types of cold viruses: rhinovirus, coronavirus, and respiratory syncytial virus (RSV) and parainfluenza. To complicate matters, RSV is included in the Northern Ireland monitoring of seasonal flu.
Can flu be prevented?
Good personal hygiene is encouraged to prevent the transmission of viruses. Avoid touching the eyes, nose or mouth; frequent hand washing (with soap and water, or alcohol-based hand rubs); covering coughs and sneezes with a tissue or sleeve; avoiding close contact with sick people; and staying home when sick.
Flu vaccine programmes aim to protect against infection by influenza viruses and reduce sickness, medical visits, hospitalisations, and deaths.
The World Health Organisation’s Global Influenza Surveillance and Response System makes recommendations for two different influenza vaccine formulations every year: one for the northern hemisphere (made in February/March), and one for the southern hemisphere (September/October). The three or four strains of influenza (H1N1, H3N2, and often two Type-B strains) most likely to attack during the next winter are chosen for inclusion in the vaccine. Influenza viruses evolve quickly, and one year’s vaccine is likely to be less effective the following year.
Every autumn, the flu vaccine is offered to people in Northern Ireland who are:
- pregnant;
- aged 65 or over;
- have an illness or underlying health condition (including children from 6 months of age);
- pre-school children aged two years and over;
- children at primary school and in the first year of secondary school (year 8);
- live in a residential or nursing home;
- people who care for an elderly or disabled person;
- frontline health and social care workers who provide direct patient care.
The 2020/21 flu vaccination programme was expanded to cover:
- 50-64 year olds;
- household contacts of those who received shielding letters during the COVID-19 pandemic;
- staff in independent care homes.
The Public Health Agency (PHA) in Northern Ireland reports that the flu vaccine uptake in 2020/21 was higher than in 2019/20. Uptake figures for 2021/22 were not available at the time this article was published.
How is seasonal flu monitored?
The PHA has a sophisticated evidence-gathering process in place to monitor the level of influenza in Northern Ireland each year. The number of General Practice and out-of-hours consultations for flu or flu-like illnesses are automatically extracted from health IT systems. Patient samples – usually nose and throat swabs – are sent for testing. This testing is enhanced by additional samples taken by 36 ‘Sentinel’ flu-spotter GP practices, which feed into Northern Ireland and UK-wide surveillance programmes.
Seasonal flu levels in 2020/21
Between one year’s week 40 and the next year’s week 20 (October through to mid-May), the PHA publishes a weekly/fortnightly Influenza Weekly Surveillance Bulletin.
According to the last bulletin of the 2020/21 season (Weeks 19–20), from 28 September 2020 through 23 May 2021, no flu — or more general respiratory — outbreaks have been reported in Northern Ireland, and just one patient was admitted to ICU with confirmed influenza (in November 2020).
Chart 1. Number of samples tested for influenza and proportion positive, 2019/20–2020/21, all sources.
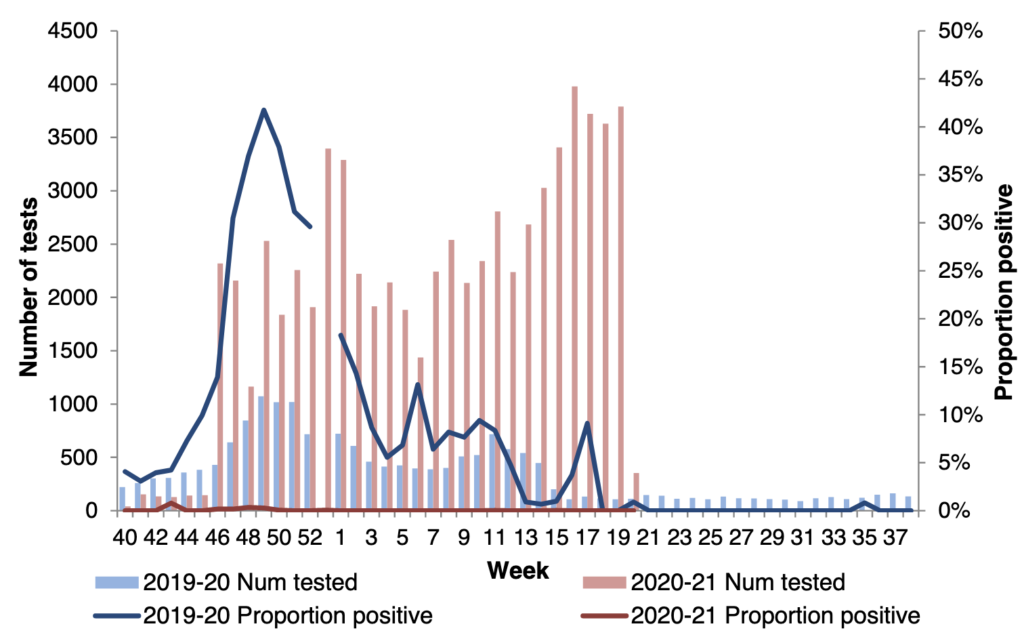
General Practice and out-of-hours consultation rates for flu are lower than 2019/20. While the number of samples being tested has increased during 2020/21 (as the regional virology lab is testing for both influenza and COVID-19), the proportion of positive results is very low compared with 2019/20, as suggested by the chart above.
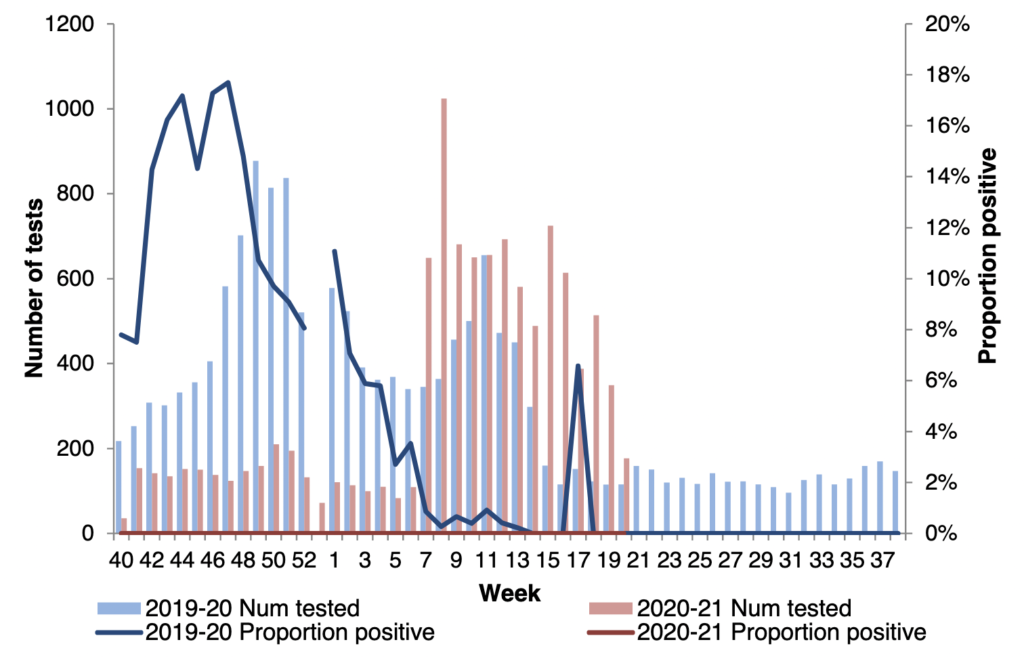
In contrast with previous years, there is a zero rate of respiratory syncytial virus (RSV; a cold virus) being detected in tested samples, as suggested by the chart below.
Chart 2. Number and samples tested for RSV and proportion positive, 2019/20–2020/21, all sources
Excess winter mortality
In this part of the world, the northern hemisphere, seasonal flu is prevalent in the winter season. This contributes to additional deaths each winter. The Northern Ireland Statistics and Research Agency (NISRA) calculates an “excess winter mortality” (EWM) figure, which compares the number of deaths that occurred in a winter period (December through to March) with the average number of non-winter deaths occurring in the preceding August to November and the following April to July.
The most recent excess winter mortality figures are for 2020/21 (charted below).
Chart 3. Deaths before, during, and after winter 2020/21
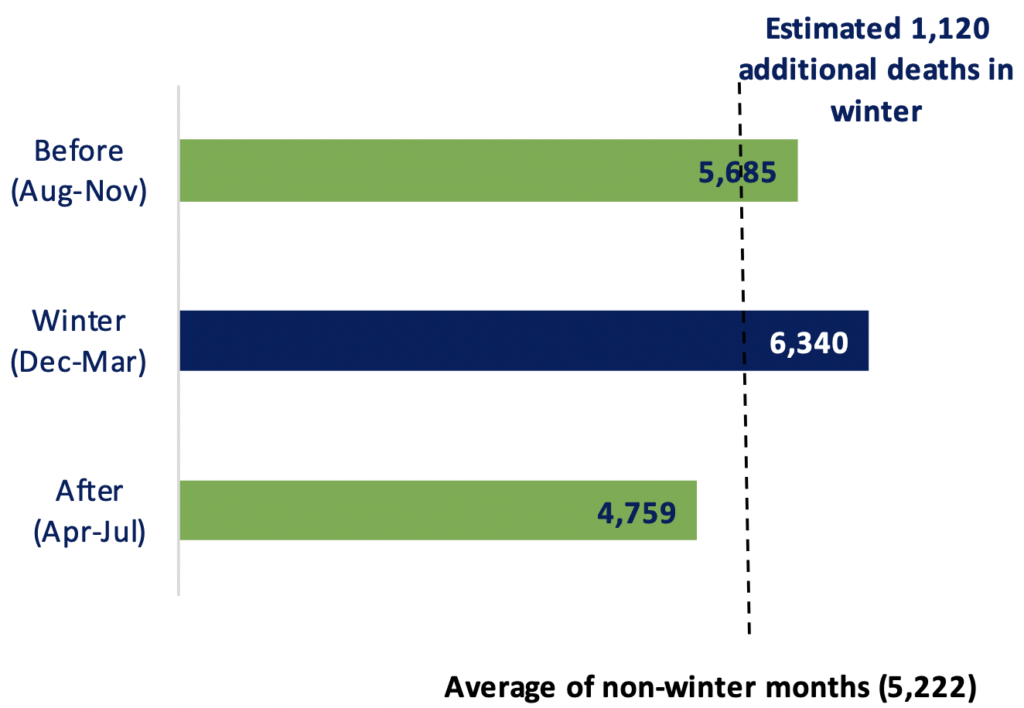
NISRA’s analysis concludes that the EWM for winter 2020/21 was approximately 1,120. The five-year moving average of excess winter mortality was 968 in 2018/19 (based on years 2016/17 to 2020/21). NISRA notes that “there has only been one higher EWM in the last 20 years (2017/18 at 1,620)”.
By removing from their analysis all deaths where COVID-19 was the underlying cause of death (while noting that we can’t know which of such deaths would have occurred regardless of the pandemic), NISRA can approximate what the excess winter mortality would have been if the current pandemic had not happened.
Chart 4. Deaths (excluding deaths from COVID-19) before, during, and after winter 2020/21
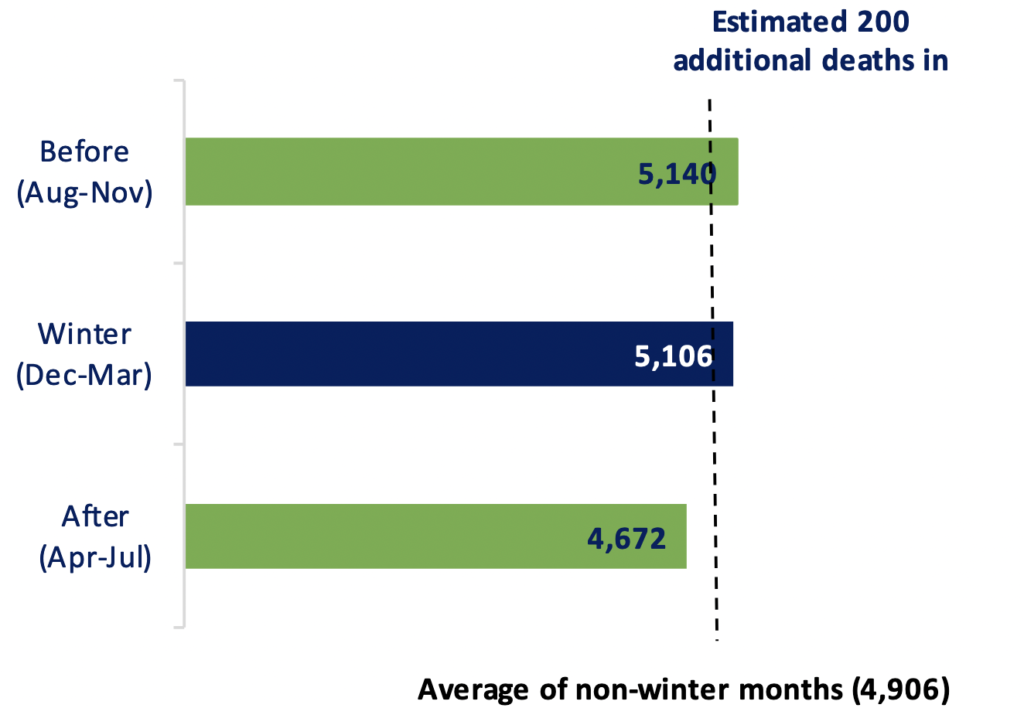
By excluding such COVID-19 deaths, the excess winter mortality for 2020/21 decreases to 200, “the lowest in EWM records”. NISRA adds: “The effect of COVID-19 has been to inflate the number of deaths in winter months, whilst not inflating the non-winter months either side to the same scale. This is [a] similar impact we’ve seen when influenza epidemics have taken hold.”
Excess Winter Mortality (EWM) that is explained above is distinct from “excess deaths”, which we explain in a separate article.
This article was originally published on 16 February 2021.
FactCheckNI is Northern Ireland’s first and only dedicated independent fact-checking service and a verified signatory to the International Fact-Checking Network’s Code of Principles. You can learn more about about FactCheckNI, our personnel, what our article verdicts mean, and how to submit a claim.




